Doctor's Diary - Infant Air Transfer on ECMO
“As an international patient transfer team, we have overcome many challenging and complex scenarios. Last month, we undertook one such clinically and logistically challenging mission: mobilizing a patient on ECMO (Extracorporeal Membrane Oxygenation). The challenge was manifold because the patient was a 6-month-old baby.
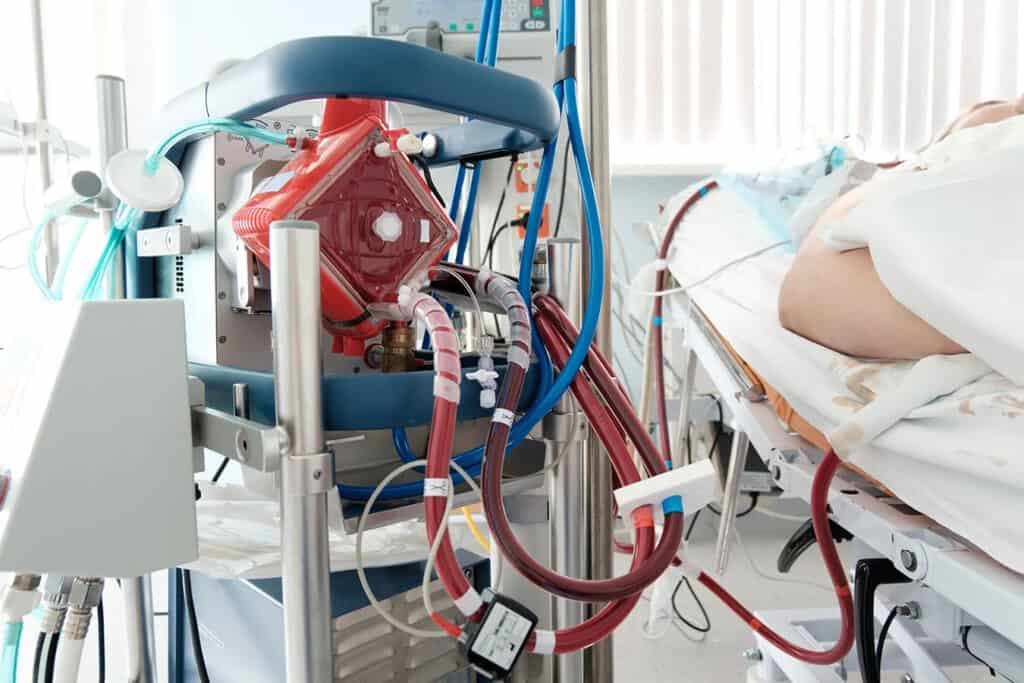
What is ECMO?
Extracorporeal Membrane Oxygenation (ECMO) is a life support machine. People who need ECMO have a severe and life-threatening illness that stops their heart or lungs from working properly
In ECMO, blood is pumped outside of your body to a heart-lung machine that removes carbon dioxide and sends oxygen-filled blood back to tissues in the body. Blood flows from the right side of the heart to the membrane oxygenator in the heart-lung machine, and then is rewarmed and sent back to the body.
This method allows the blood to “bypass” the heart and lungs, allowing these organs to rest and heal. Thus ECMO is used in critical care situations when your heart and lungs need help so that you can heal. It may be used in care for COVID-19, ARDS, heart failure, etc.
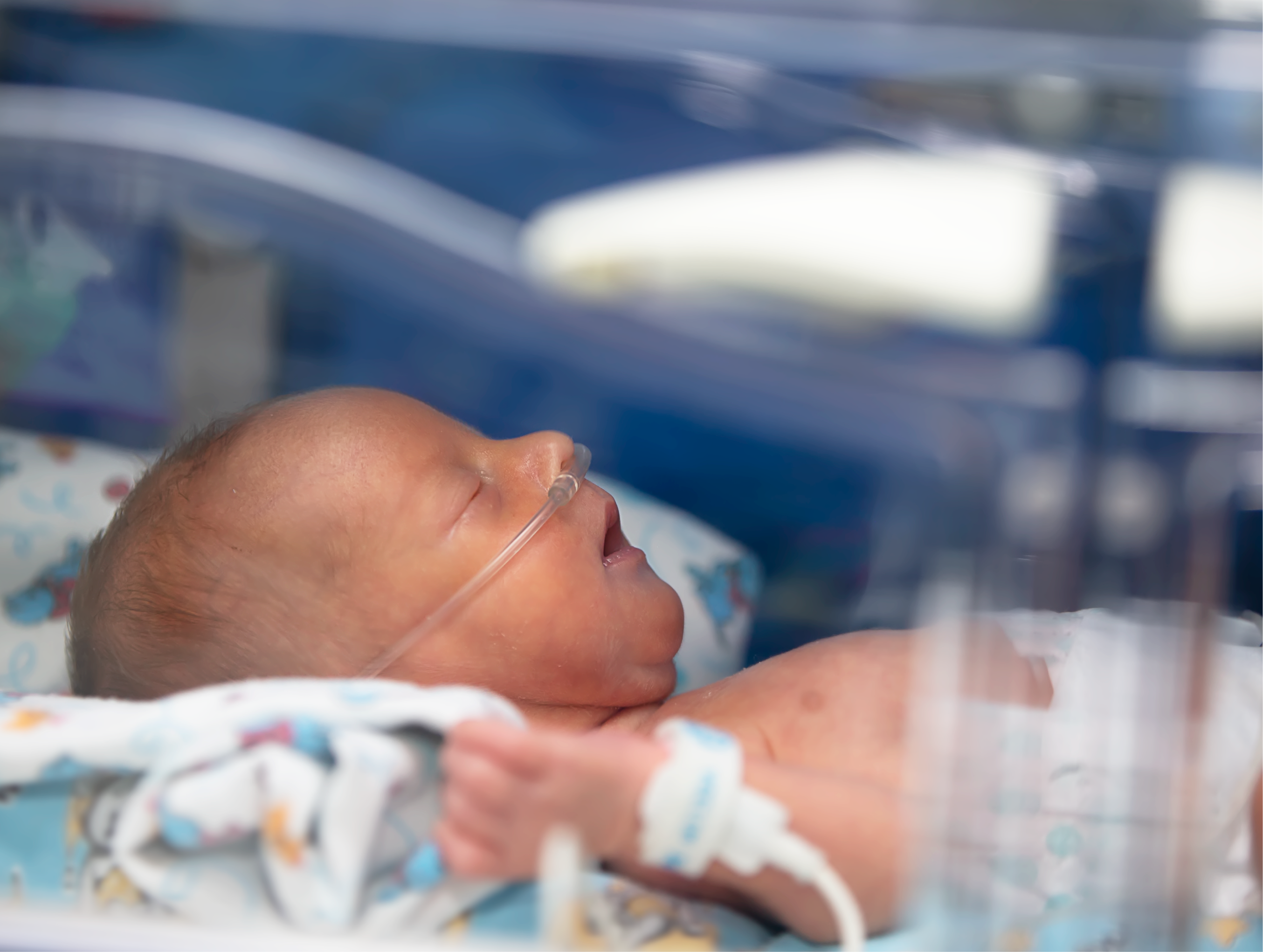
The 6-Month Old Patient
The patient presented to us was a 6-month-old female, whose heart was failing due to yet unknown reasons, and was in need of a heart transplant urgently. The baby was on multiple life support at the time of our evaluation and was under multidisciplinary care. And after careful evaluation, we briefed the treating team regarding the risk of her transportation via air because of the complexity of care that she needs during such a transfer.
However, the lack of transplant facilities in the region made it a situation where the benefits outweighed the risks. We were informed by the intensive care team that they have plans for initiating ECMO on the patient for getting her more stable. We, as a transport team, concurred since it would give us better control of the patient’s hemodynamics which in turn will reduce the risk of the transfer.
ECMO was initiated on the baby by the cardiothoracic team, in a complex procedure of opening up the chest and inserting tubes to pump blood to the machine outside the patient’s body. While the ICU team was working hard to get the baby stable in the ICU, our flying ECMO team was making arrangements to transfer the baby to an alternate facility for continued care. After multiple discussions, team meetings, and arranging the necessary transport devices for such a complex transfer, our team was given permission to take the baby out of the ICU.
Advantage Cessna
The amount of space inside the aircraft was a crucial factor here, due to two major reasons: the number of people onboard and the number and size of equipment needed for care. An ECMO transfer team consists of a 4-person medical team – a pediatric intensivist, a PICU nurse, a Perfusionist, and a Flight Physician. Since the patient was a baby, one of the parents had to be on board.
Besides that, multiple equipment, including a ventilator, ECMO machine, syringe pumps, multipara invasive monitoring, suction apparatus, emergency responder kit, etc were needed onboard. Thanks to our Cessna Citation Sovereign C680 with a bigger cabin volume, extra seating, and more cabin height to work around, we were able to overcome all the above-mentioned limitations of space for this transfer.
After a week of meticulous planning and preparation, the baby was finally flown out to an alternate facility for continued care. Other than the expected complexity of care for such a case, the journey onboard was uneventful, and the baby was handed over to the receiving team in the same clinical status as she was from the original facility. Our wishes and prayers for the baby and her family. May she have a quick clinical recovery and come out of the hospital in a stable state of health.”
Dr. Afsal Mohammed
Medical Director